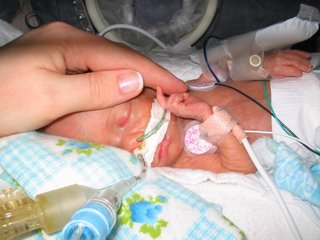
Lots of people ask me about Aiden's stay in the NICU. I am transcribing his NICU Discharge Summary for those people, for those of us who lived through it and will be surprised to be reminded of the extent of what transpired and for people who are going through a similar experience. Aiden is a beautiful example of the fact that a tiny little baby can survive an awful lot.
Discharged Date: 2005 June 1
DISCHARGE DIAGNOSES:
1. Prematurity.
2. Intrauterine growth restriction.
3. Bronchopulmonary dysplasia.
4. Respiratory distress syndrome.
5. Patent ductus arteriosus [closed].
6. Retinopathy of prematurity.
7. bilateral inguinal hernia.
8. Feeding incoordination.
9. Intraventricular hemorrhage.
ONGOING ISSUES:
1. Feeding difficulties.
2. Bronchopulmonary dysplasia.
3. Postoperative follow-up of inguinal hernia repair.
PRENATAL HISTORY: Baby McKerracher was born to a healthy 32-year-old G2 P1 woman from xxx (city withheld). Early in the pregnancy, the maternal serum screening test was drawn and showed some abnormalities consistent with potential Down syndrome. An amniocentesis was performed at 19 weeks which has shown to be normal with normal chromosomal count. Other routine prenatal blood work was negative. The ultrasound performed at 20 weeks gestation, however, showed the first signs of grown restriction. Form 20 weeks on, Baby McKerracher was exhibiting increasing size; however, given his gestational age, he was found to be consistently smal lfor gestational age.
LABOUR AND DELIVERY: At 27 weeks gestation, there was a spontaneous rupture of membranes. At this time, Baby McKerracher underwent a biophysical profile which was found to be a 1/10. This was also associated with continually increasing maternal blood pressure. Because of these findings, it was decided that he should be delivered by C-section urgently. His mother did receive one dose of Celestone several hours before the delivery. The membranes were only ruptured for approximately eight hours. the GBS status was unknown. there was no sign of maternal fever or sepsis at the time. The baby was delivered by C-section and did quite well initially. He emerged quite vigorous, though very small. the Apgars were reported to be 8 at 1 minute and 9 at 5 minutes. He was initally given suction and oxygen by positive pressure ventilation. He was found to have increased work of breating at birth and was intubated and given one dose of Surfactant which did seem to improve his work of breating at the time. Shortly after delivery, he also had umbilical artery and umbilical venous central lines placed.
On initial physical exam, Baby McKrracher's birthweight was noted to be 550 gm, head circumference 23 cm and length 31 cm. All of these measurements placed him greater than two standard deviations below the mean. Despite being extremely small for gestational age, there was n other significant abnormalities noted on the initial physical exam for Baby McKerracher. However, a gestational maturity was assessed using the Ballar Scoring System and he was found to be roughly 24 weeks in matureity at the time of birht.
COURSE IN HOSPITAL: Baby McKrracher was born quite premature and spent a long and eventful time in the Neonatal Intensive Care Unit. He did suffer most of the many complications affilated with prematurity. The following is a summary of his course by system:
Nutrition, Fluid and Electrolytes: We did have some significant difficulty in establishing feeds with Baby McKerracher. He was placed on TPN on the second day of life, and he remained on TPN for 73 days in total. He did suffern from some evidence of TPN cholestasis. While trying to establish feeds, he did recieve mostly expressed breast milk by NG tube. We did experience some difficulty in trying to get him to feed via nipple. the Feeding Team at the Child Development Center was involved and had made some recommendations. We eventually were able to get him feeding with the nipple by providing him wiht some thickened feeds. At the time of discharge, Baby McKerracher was being closely followed by the Feeding Team and was thriving on entirely nippled feeds consisting of thickened NeoSure. Baby McKerracher was sent home on this thickened formula, and he wil lbe followed up by the Feeding Team. During his stay in hospital, he also did suffer from some of the typical electrolyte fluctuatiopns seen with prematurity, though there was no significant problems associate with this. His electrolytes were all normal at the time of discharge.
RESPIRATORY: Baby McKerracher was diagnosed with respiratory distress syndrome at birth and received two doses of Surfactant. Unfortunately, he want on to develop severe bronchopulmonary dysplasia. He had suffered from many complications from his BPD and had several significant desaturations requiring manual ventilation and high oxygen content. Because of his very volatile BPD, we did have him intubated for an extended period of time. He spent a total of 77 days intubated. He also received six days of intravenous Hydrocortisone in order to help stabilize his lungs. While in hospital, he was also treated for his BPD with Lasix. He spent approximately 70 days in hospital while on Lasix. He also received inhalers which he was still taking at the time of discharge. Following extubation, Baby McKrracher was weaned down to a minimul amount of low flow oxygen. We were unable to remove the oxygen entirely, and he was sent home with oxygen. He was requiring roughly 0.01 L/minute of low flow oxygen. At the time of discharge, he was quite stable on this minimul amount of low flow oxygen; however his blood gases inducated that he was a cronic C02 retainer with consisten capillary gas values of 70 mmHg.
CARDIOVASCULAR: Shortly after birth, physical exam indicated that Baby McKerracher had a murmur. An echocardiograph was performed which indicated the presence of a moderate PDA. Because of his extreme prematurity and the fact that he was also mildly symptomatic from this, it was decided to close the PDA via Indomethacin. He received one three-day course of the Indomethacin which closed the PDA successfully on follow-up echo. At the time of discharge, there was nothing to indicate on physical exam that the PDA had reopened. It should also be noted that Baby McKerracher did suffer from some significant episodes of desaturation resulting in bradycardia. He had one particular episode where he required chest compressions due to poor saturations which persisted for up to 10 minutes. He reuqired Epinephrine on this one occasion. (Nicole's note: Ric and I were actually in the NICU with Aiden when he had this one "episode." And, it was probably the strangest, scariest and most profound half hour of my life.) He also required chest compressions on three additional occasions.
GASTROINTESTINAL: Baby McKerracher did take quite a long time in order to establish oral feeds. Fortunately, ther ewas no evidence that he suffered from any necrotizing enterocolitis. He did develop an indirect hyperbilirubinemia at birth which was treated with phototherapy. The highest indirect bilirubin level was measured to be 198. He did not need any exchange transfusions for this. He also developed a component of TPN cholestasis. the maximum direct bilirubin that he achieved was 127. At the time of discharge his direct bilirubin was decreasing consistently. He did also have elevated liver enzymes which also were showing a decreasing trend. A the time of discharge, he was feeding and stoolign well without any significant problems. While in hospital, it was also noted that Baby McKerracher had bilateral inguinal hernias. He had these repaired surgically by Dr. Sarah Jones on May 17. He tolerated this quite well. He was also noted to have gastroesophageal reflux shortly prior to his discharge. He was placed on Maxeran and Ranitidine in order to help treat this problem.
NEROLOGICAL: On routine head ultrasound, it was found that Baby McKerracher suffered from intraventricular hemorrhage. In the end, he was found to have grade IV hemorrhage on the left side, and there were some mention made of potential periventricular leukomalacia. He also had grade I-II hemorrhage on the right side. Fortunately, he did not suffer any seizures while in hospital. It was also noted that at discharge, did did have a relatively normal neurologic exam with appropriate tone and limb movement. The one significant neurologic symptom that we were able to observe was some feeding incoordination.
INFECTIOUS DISEASE: Baby McKerracher suffered from three episodes of severe sepsis. One of these episodes was likely pneumonia. The others were confirmed bacteremia with positive cultures of Staphylococcus epidermidis. During one of these episodes, he also suffered from disseminated intravascular coagulation. He spent a lot of time of antibiotics while in NICU. These included 10 dyas on Gentamicin, 30 days on Vancomycin and 22 days on Amphotericin. These episodes of sepsis made Baby McKerracher critically ill and one of them was associated with significant desaturation requiring chest compression and Epinephrine. At the time of discharge, he had recovered from all of these episodes of sepsis.
RENAL: Baby McKerracher did suffer from some transient elevation of creatinine and BUN in association with episode of sepsis likely due to prerenal failure. At the time of discharge, his creatine and BUN had normalized, and he had maintained good urine output. It should be noted, however, that he was exposed to many nephrotoxic medications for prolonged periods of time during his stay.
HEMATOLOGICAL: Because of his prematurity and the episode of DIC, Baby McKerracher did require several transfusions. In the end, he ended up getting nine transfusions of packed red cells and six transfusions of platelets. The packed red cell transfusions were donated from his father. At the time of discharge, his blood counts had normalized with hemoglobin 106, platelets 320, white cells 12.4, and a high reticulocyte count.
OPHTHALOMOLOGICAL: Baby McKerracher did suffer from some significant retinopathy of prematurity and was followed by Ophthalmology while in hospital. His ROP reached stage III zone II in the right eye and the left eye. He was treated with laser retinopexy on April 12 by Dr. Dale. This was tolerated quite well with no complications. On follow-up examination, it was noted that hde did get extremely good results from the surgery with resolving retinopathy. It was noted that he had some mild residual tortuosity of his vessels and immature macular development. He wil lb efollowed up by Ophthalmology post discharge.
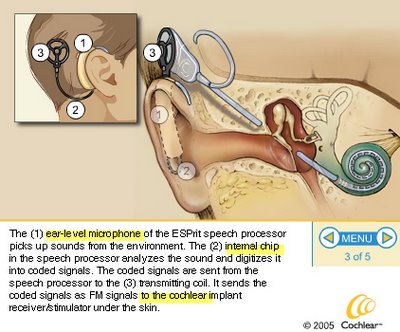
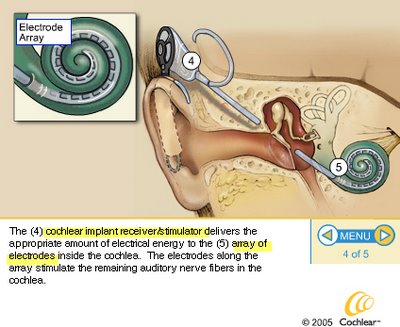
HEARING: Baby McKerracher had a hearing test, which was inconclusive just prior to discharge. He had been exposed to several ototoxic medicatons and this test should be followed up. There has been a repeat testing booked.
VACCINES: While in hospital, Baby McKerracher received one dose of Prevnar and Pentacel vaccines. Obviously, his caccination schedule has been delayed significantly.
DISCHARGE PHYSICAL EXAM: At the time of discharge, Baby McKerracher looked well and was stable on a small amount of low flow oxygen. His weight was 2735 gm (6 pounds), length 47 cm and head circumference 36.5 cm. He was noted to have a relativelty normal neurologic exam. His red reflexes were present bilaterally. There was no murmur heard. His vital signs were all within normal limits. the palate was intact. The hips were normal. Testes were descended bilaterally with normal male genitalia.
SUMMARY: Baby McKerracher was born prematurely with intrauterine growth restriction. He spent 5.5 months in the NICU and did suffer from many complications associated with prematurity. He spent much of his time critically ill and did require many emergency interventions during that time. Fortunately, during the last month-and-a-half in hospital, he has gotten over his major problems and was gaining weight on his thickened formula. Obviously, there will be need for some close follow-up from everal differnt people for him. He will be seen by Dr. Dempsey in Belleville for regular care. He wil also be seen at Special Infant Clinic and at the Child Development Center for the Feeding Team. He will also be seen by Ophthalomology in two months' time and be followe up by Dr. Sarah Jones for evaluation of his hernia repair. He will also be seen for repeat of his heraing exam.
DISCHARGE MEDICATIONS:
1. Elemental iron 7.7 mg qd.
2. Tri-Vi-Sol 0.5 ml qd.
3. Atrovent two puffs bid.
3. Ventolin two puffs bid.
5. Flovent 125 mcg two puffs bid.
6. Maxeran 0.25 mg q. 8h.
7. Ranitidine 3.8 mg bid.
8. Low Flow oxygen.